What are motility disorders?
Motility disorders occur when the nerves and muscles in the gastrointestinal (GI) tract fail to work together properly.
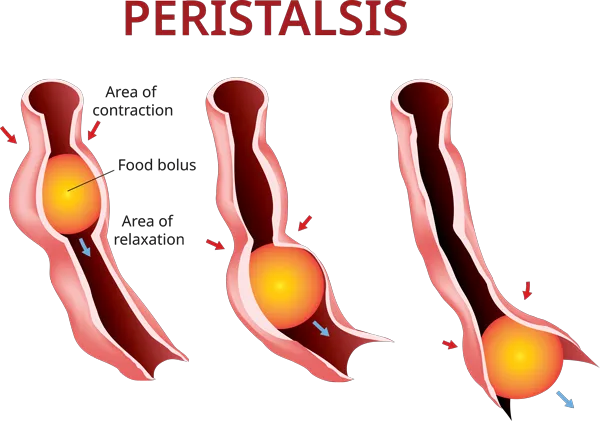
During normal digestion, food is pushed through the digestive tract in a series of coordinated wave-like movements called peristalsis. The muscles living your intestinal tract involuntarily contract and relax in this coordinated fashion, pushing food forward from your esophagus to your stomach, all the way through your small intestines and large intestine to your rectum and anus.
In a motility disorder, these contractions don't occur in a coordinated fashion. The result is food not passing through your digestive tract in a timely or proper way.
Any change in how food is moved along the digestive tract may be considered a motility disorder.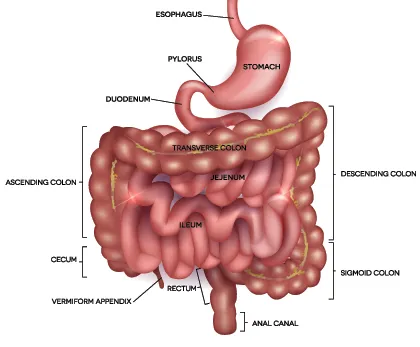
What Causes Motility Disorders?
Motility disorders occur:
- As a result of problems with the nerves and/or hormones that control the muscle of the GI tract,
- Due to problems with the intestinal muscles themselves responsible for peristalsis, or
- Due to a problem with how the nerves and muscles work together to produce peristaltic waves.
When muscle contractions don’t occur in a coordinated fashion motility disorders result
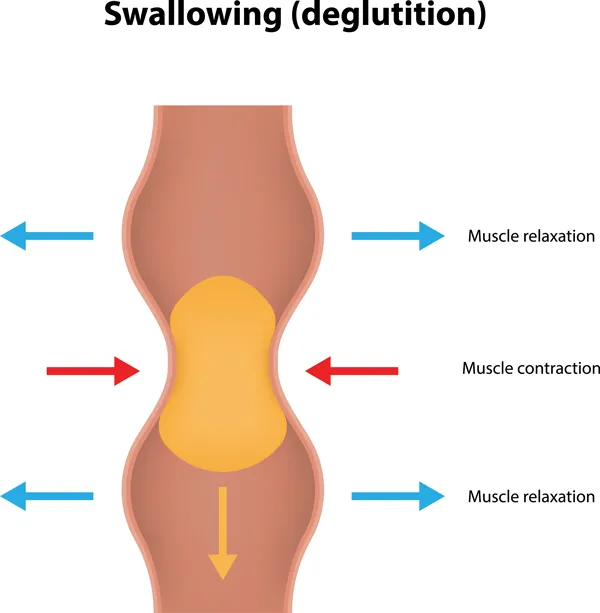
Sometimes medications may interfere with intestinal motility. Endocrine disorders like severe hypothyroidism and diabetes can also affect GI motility.
What are the symptoms of motility disorders?
Symptoms vary widely depending upon the part of the GI tract affected, but they may include:
- Severe constipation (meaning bowel movements that are infrequent or hard to pass),
- Fecal soiling or incontinence,
- Diarrhea and/or passing undigested particles of food in your stool,
- Gas, bloating, abdominal distention, stomach swelling
- Abdominal pain or discomfort,
- Nausea or vomiting,
- Reflux or GERD symptoms,
- Regurgitation of food contents,
- Difficulty swallowing,
- The sensation of food getting stuck or food actually getting stuck in the esophagus,
- Choking
How are Motility Disorders diagnosed?
A variety of tests may be used to help formulate the diagnosis, and may include:
- Manometry studies: These tests measure the pressure in different areas of your GI tract. Esophageal manometry specifically measures the contractions in your esophagus during swallowing.
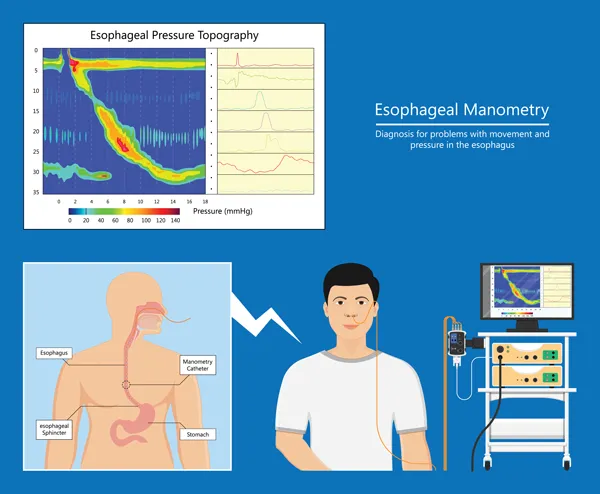
- Esophogram is an x-ray of your esophagus taken after swallowing a substance like Barium used to highlight your esophagus.
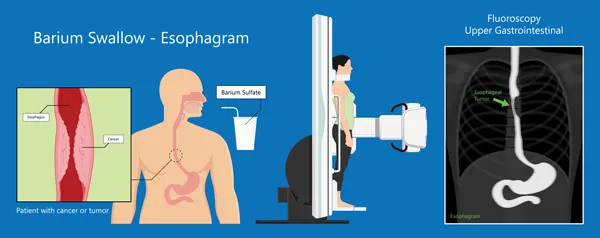
- Upper GI series: is a series of x-rays taken of the upper GI tract (including the esophagus, stomach, and duodenum) after swallowing a substance like Barium used to highlight or enhance the structures.
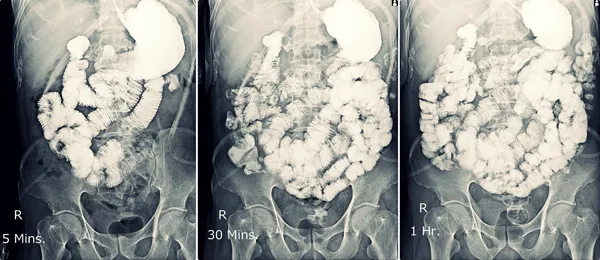
- Gastric emptying studies: use nuclear medicine to determine how quickly food leaves your stomach. A small amount of radioactive material is used to emit photon energy. It’s different than a basic x-ray which doesn’t use nuclear medicine.
- Sitz marker tests for colonic transit time: estimate how long it takes for food to move along your colon. You ingest radiopaque markers. Then, x-rays of your abdomen are taken to see how long it takes you to clear the markers from your colon.
- 24-hour pH impedance testing: measures the amount of reflux (both acidic and nonacidic) in your esophagus during a 24-hour period of time, and assesses whether your symptoms correlate with the reflux or not.
What are the different types of Motility Disorders?
There are a number of different motility disorders. Examples include:
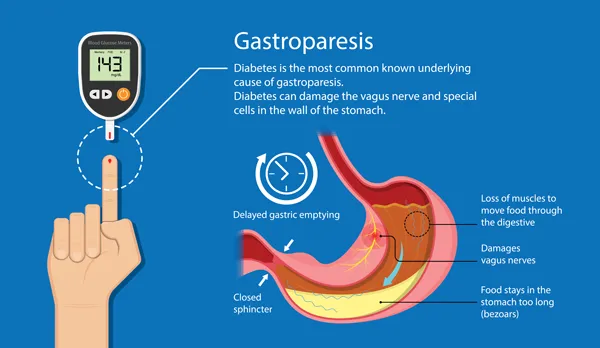
- Gastroparesis or "delayed gastric emptying".
- This is when food stays in your stomach for longer than it should.
- Diabetes is the most common cause of gastroparesis. High blood sugar levels damage the nerves in your stomach and prevent your stomach muscles from contracting and relaxing properly
- When food moves too slowly out of your stomach and into your intestines symptoms like nausea, vomiting, belching, bloating, heartburn, indigestion, and regurgitation of food contents may occur
- Irritable Bowel Syndrome (IBS) or spastic colon is a diagnosis that describes a cluster of symptoms including repeated episodes of abdominal pain, often relieved by a bowel movement, and changes in your bowel habits, such as diarrhea, constipation, or both. IBS is considered a "functional" disorder of the digestive tract, meaning it affects how your digestive tract functions but it doesn't damage the organs themselves. When you have IBS, your digestive motility can be altered. If food moves too quickly through your digestive tract, diarrhea, excess mucus, and the passage of undigested food particles can result. If food moves too slowly, constipation can result

- Esophageal Spasms are irregular contractions of the muscles in your esophagus, the long muscular tube that carries your food from your mouth to your stomach. This can cause severe pain and spasms in your esophagus and/or chest, a feeling as if something is stuck in your throat and/or chest, difficulty swallowing, heartburn, an acid taste in the back of your throat, regurgitation of food or liquid back up into your mouth, and even sometimes the sensation of heart palpitations. Cardiac and other causes must always be ruled out due to the similarity in symptoms between esophageal spasms other life-threatening conditions.
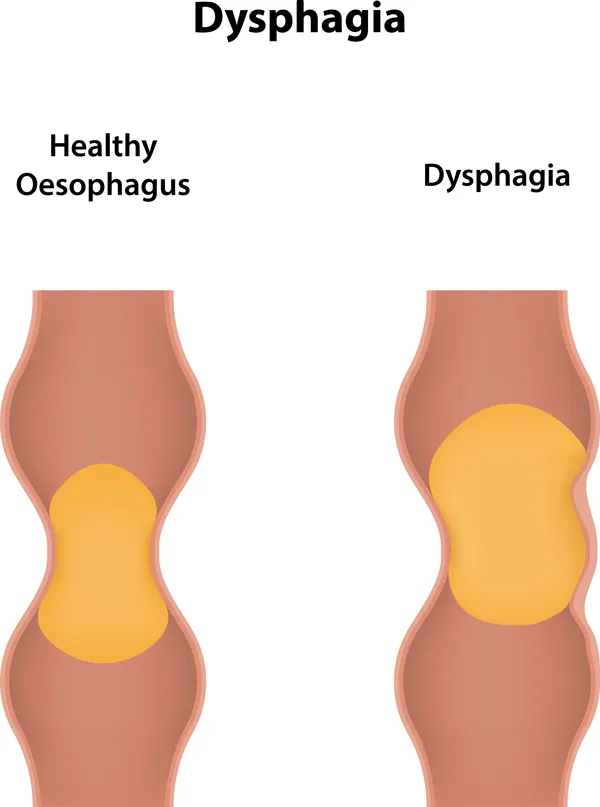
- Dysphagia is a general term for difficulty swallowing. While swallowing may seem very involuntary and basic, it’s actually a rather complex process involving many different muscles and nerves. Difficulty swallowing can develop due to multitude of reasons including motility problems.
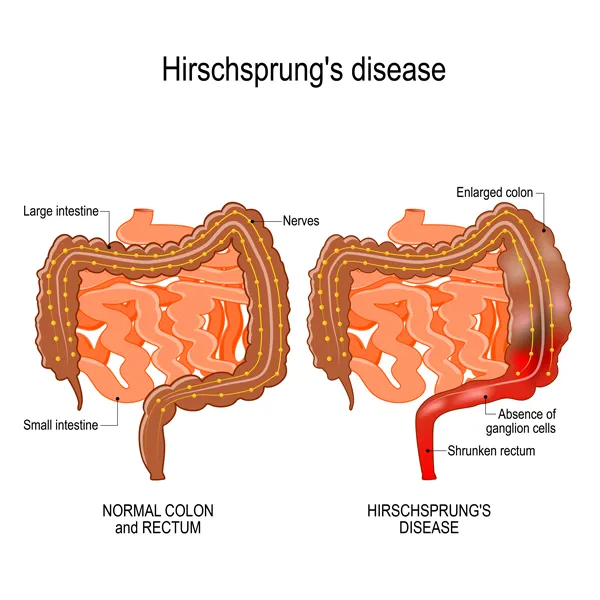
- Hirschsprung's Disease or congenital aganglionic megacolon is a congenital disorder that occurs when intestinal nerve cells don’t develop properly during fetal development. Cells in the large intestine lack nerve cells required to cause the colon to relax and the colon become blocked with stool. Babies become severely constipated. The condition is present at birth.
- Fecal incontinence is when you’re unable to control your bowel movements, causing feces to leak out from your rectum. Fecal incontinence can range from occasional leakage to total loss of bowel control. Causes may include: neurologic disorders, stroke, spinal cord injuries, rectal tears during childbirth, surgical complications from rectal and anal surgeries, benign or malignant masses pushing on the intestinal tract, overflow diarrhea (secondary to severe constipation), and certain foods and artificial sweeteners. Lactose deficiency can trigger uncontrollable diarrhea and subsequent fecal incontinence. Some long-distance runners will describe a condition known as Runner’s diarrhea that can lead to embarrassing fecal incontinence while running.
- Constipation occurs when bowel movements become less frequent and stools become difficult to pass. Causes include: not enough water in the diet, a diet low in fiber and high in animal fats and processed foods, pregnancy, ignoring the natural urge to defecate (and “holding it”) due to work/life situations, or sometimes due to painful conditions like anal fissures, large obstructing hemorrhoids, hypothyroidism, electrolyte imbalances, hormonal imbalances, and benign or malignant masses pushing on the intestinal tract.

- Scleroderma or systemic sclerosis, is a chronic autoimmune disease, that involves a hardening or tightening of the skin and connective tissues. It also can affect your digestive tract and result in problems with swallowing and other motility issues.
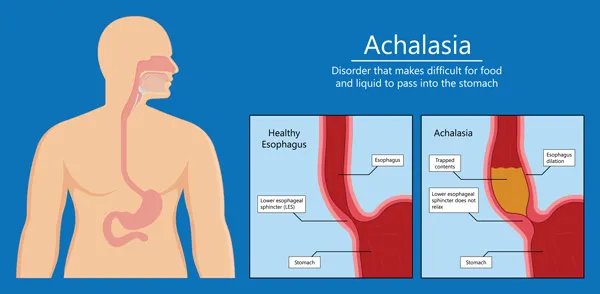
- Achalasia involves the ring of muscle at the very bottom of your esophagus called the lower esophageal sphincter or LES. The LES closes off your esophagus from your stomach and prevents food from coming back up into your esophagus once it gets into the stomach. With achalasia, your LES fails to relax properly during swallowing. Food doesn't move as easily from the esophagus into your stomach and it backs up in your esophagus. Symptoms may include chest pain, regurgitation of food or food particules, heartburn, difficulty swallowing, and difficulty belching or painful belching.
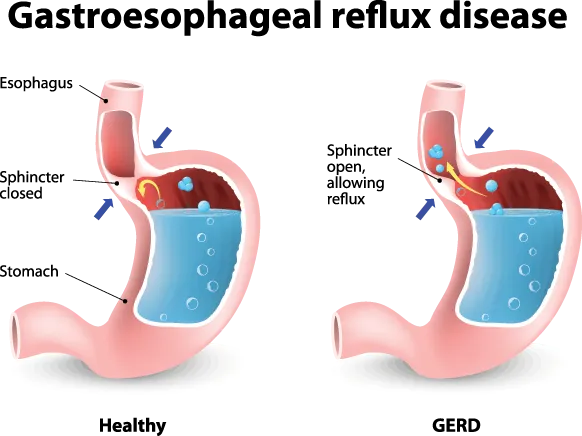
- GERD or Gastroesophageal reflux disease< is a longstanding condition where acid from your stomach consistently refluxes back up into your esophagus and damages the lining of your esophagus. GERD is considered a motility disorder involving the lower esophageal sphincter or LES. The LES relaxes too much allowing your stomach contents to reflux back up into your esophagus and damage the lining of your esophagus.
How common are Motility Disorders?
In depends on the specific disease. Some motility disorders are more common than others. Statistics suggest 30-45% of all GI conditions could be classified as a motility disorder.
What are the Risk Factors for Motility Disorders?
Risk factors vary based on the specific condition.
For example, individuals with Diabetes are at increased risk for Gastroparesis. Having certain neurological disorders like MS, ALS, Parkinson’s disease, Myasthenia Gravis, or a history of stroke or central nervous system disease may increase your risk of other motility disorders. IBS can be triggered by infection. This is known as post-infectious IBS. Other motility conditions carry a genetic component.
What are the Treatment Options for Motility Disorders?
Treatment is dependent upon the exact diagnosis but may include medications, pelvic floor physical therapy, biofeedback programs, pacemakers, and more invasive surgical interventions.
What are the complications of motility disorders?
Complications of intestinal motility disorders vary greatly depending on the specific disorder. Examples of complications may include:
Impaction, in the case of severe constipation. Impaction is the build up of dry and hardened feces in the rectum or colon. Symptoms may include: abdominal pain, rectal pressure, vomiting, overflow diarrhea, dehydration, confusion, change in mental status, fever, chills, and sweats.
Complications of fecal incontinence may include recurrent urinary tract infections, sepsis, and psychological problems related to the embarrassing nature of the condition.
Complications of esophageal dysmotility may include aspiration pneumonia, food impaction, and choking.
IBS is not usually associated with complications.
